
When it comes to protecting your heart, most people immediately think about cholesterol or blood pressure. But there’s another key player that often goes overlooked: insulin resistance. Understanding what insulin resistance is- and how it connects to heart health- can be an empowering step toward making choices that keep your whole body healthier for years to come.
What Is Insulin Resistance?
Insulin is a hormone made by your pancreas that acts like a “key,” allowing sugar (glucose) from the food you eat to move out of your bloodstream and into your cells, where it’s used for energy.
With insulin resistance, the body’s cells don’t respond as effectively to insulin’s signal. Imagine the “lock” on the cell has become rusty and the insulin “key” doesn’t fit as smoothly anymore. As a result, your body has to produce more insulin to get the same job done.
Over time, this can cause:
- Higher insulin levels in the blood (called hyperinsulinemia)
- Higher blood sugar levels (since glucose isn’t entering cells as easily)
- Extra strain on the pancreas, which works overtime to keep up
If the pancreas can’t keep up with the demand, blood sugar levels rise further, often leading to prediabetes or type 2 diabetes.
What Causes Insulin Resistance?
Insulin resistance develops slowly over time and is influenced by a variety of factors, including:
- Excess body fat, especially visceral fat (around the waist). Belly fat is metabolically active and can release inflammatory signals that interfere with insulin’s job.
- Physical inactivity. Regular movement helps muscles take in glucose more effectively. Without it, insulin has to work harder.
- Diet high in refined carbs and added sugars. These foods cause blood sugar spikes that put stress on insulin pathways.
- Chronic stress and poor sleep. Both raise hormones that can worsen insulin resistance.
- Genetics and family history. Having relatives with type 2 diabetes or metabolic conditions increases risk.
- Hormonal changes. Conditions like polycystic ovary syndrome (PCOS) are strongly linked to insulin resistance.

How Does Insulin Resistance Impact Heart Health?
Insulin resistance isn’t just about blood sugar—it affects the entire cardiovascular system. Here’s how:
- High blood sugar damages blood vessels. Over time, this can stiffen arteries and reduce their flexibility, making it harder for blood to flow.
- High insulin levels promote fat storage. This often leads to weight gain around the abdomen, which raises the risk of heart disease.
- Cholesterol and triglycerides get out of balance. Insulin resistance is often linked to high triglycerides, low HDL (“good” cholesterol), and small, dense LDL particles—all of which increase heart risk.
- Inflammation rises. Chronic low-grade inflammation damages blood vessels and speeds up plaque buildup.
- Blood pressure creeps up. Insulin resistance contributes to fluid retention and changes in blood vessel function, both of which raise blood pressure.
The fact is, insulin resistance sets the stage for heart disease, even before diabetes develops. That’s why addressing it early is one of the best gifts you can give your heart.
Nutrition and Lifestyle Tips for Reducing Insulin Resistance
The good news is that insulin resistance is highly responsive to lifestyle changes. Even small, consistent steps can improve your body’s sensitivity to insulin and protect your heart, and these same lifestyle changes also lower your risk for cancer, dementia, and other chronic diseases that impact long-term health and longevity.
Here are some evidence-based strategies:
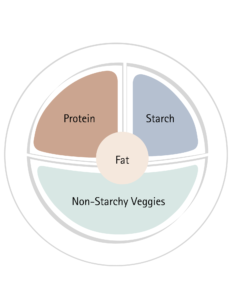
1. Prioritize Balanced Meals
- Aim for a balanced plate with protein, fiber-rich carbs, and healthy fats at each meal.
- Examples: grilled salmon with quinoa and roasted veggies, or a ground chicken, bean and veggie chili topped with avocado.
- Balanced meals help keep blood sugar steady, reducing strain on insulin.
2. Choose Quality Carbs
- Favor whole grains, beans, lentils, fruits, and vegetables.
- Limit refined carbs like white bread, pastries, and sugary drinks that spike blood sugar quickly.
3. Move Your Body Daily
- Exercise helps muscles absorb glucose without needing as much insulin.
- Aim for 150 minutes per week of moderate activity (like brisk walking, biking, or swimming).
- Add strength training 2–3 times per week to build muscle, which acts as a glucose “sponge”, absorbing glucose from the blood stream and storing it as molecule called glycogen. The more muscle you have, the greater your glucose-storing capacity.

4. Support a Healthy Weight
- Even a 5–10% weight loss (if recommended for you) can significantly improve insulin sensitivity.
- Focus on sustainable habits instead of quick fixes.
5. Get Quality Sleep
- Aim for 7–9 hours most nights. Poor sleep can raise stress hormones and worsen insulin resistance.
- Learn some tips for getting a good night’s sleep here.

6. Manage Stress
- Chronic stress raises cortisol, which can interfere with insulin.
- Try deep breathing, journaling, prayer, or short walks to reset during the day.
7. Limit Added Sugars and Processed Foods
- These foods contribute to insulin spikes and inflammation.
- Choose naturally sweet options like fresh fruit when you want something sweet.
The Takeaway
Insulin resistance is more than a blood sugar issue- it’s a powerful driver of heart disease risk. The encouraging news is that your daily choices can make a huge difference. By focusing on balanced nutrition, movement, rest, and stress management, you can improve insulin sensitivity, lower your heart risk, and feel better in your day-to-day life.
Taking care of your heart truly starts with taking care of your metabolism. Small, steady steps today add up to lifelong benefits.
